Female Fertility Tests: Understanding AMH and Antral Follicle Count to Assess Egg Reserve
When couples plan pregnancy, one of the most common questions women ask is: How can I check my egg quality? In clinical practice, egg quality cannot be measured directly. However, doctors estimate fertility potential using markers of ovarian reserve, primarily the Anti-Müllerian Hormone (AMH) test and the Antral Follicle Count (AFC) measured by ultrasound. Together, these two tests give valuable insight into how the ovaries are functioning and how they may respond to fertility treatments such as IVF. 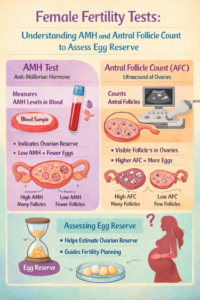
AMH Test: What It Measures and How It Is Done
AMH (Anti-Müllerian Hormone) is a hormone produced by the granulosa cells of small follicles in the ovary. Because it reflects the number of early follicles present, AMH serves as a useful indicator of remaining egg reserve.
One advantage of AMH is that the blood test can be performed on any day of the menstrual cycle, unlike some other fertility hormones. AMH levels are measured in the laboratory using immunoassay techniques, most commonly automated electrochemiluminescent or enzyme-linked immunoassays that detect the concentration of AMH circulating in the bloodstream.
Interpreting AMH Levels
Although values vary slightly between laboratories, general clinical interpretation is as follows:
- Normal AMH: approximately 1.5–4.0 ng/mL
- Low AMH: below about 1.0 ng/mL (suggesting reduced ovarian reserve)
- Very low AMH: below 0.5 ng/mL (often associated with poor ovarian response in IVF)
- High AMH: above about 4–5 ng/mL, often seen in women with polycystic ovarian morphology or PCOS
It is important to note that AMH measures egg quantity rather than egg quality, and younger women with low AMH may still conceive.
Situations Where AMH May Be Erroneously Low
AMH levels can sometimes appear lower than the true ovarian reserve in certain situations, such as:
- Recent hormonal contraceptive use
- Severe vitamin D deficiency
- Recent ovarian surgery (especially endometrioma surgery)
- Temporary suppression after pregnancy or hormonal therapy
- Laboratory variability between assay methods
Therefore, AMH results should always be interpreted in clinical context rather than used as a standalone fertility predictor.
Conditions Associated With High AMH
Elevated AMH levels are commonly seen in:
- Polycystic ovary syndrome (PCOS)
- Polycystic ovarian morphology
- Women with very high follicle numbers
In IVF practice, very high AMH may predict a strong ovarian response and potential risk of ovarian hyperstimulation syndrome.
Antral Follicle Count (AFC): Ultrasound Measurement of Ovarian Reserve
The Antral Follicle Count (AFC) is another important method used to estimate ovarian reserve. It is measured using transvaginal ultrasound, typically performed in the early follicular phase of the menstrual cycle (day 2–5).
During the scan, the doctor counts the number of small follicles measuring approximately 2–10 mm in diameter in both ovaries. Each of these small follicles represents a potential egg that could respond to hormonal stimulation.
Interpreting Antral Follicle Count
Typical ranges used in clinical practice include:
- Normal AFC: about 8–15 follicles in both ovaries combined
- Low AFC: fewer than 5–7 follicles, suggesting diminished ovarian reserve
- High AFC: more than 20 follicles, commonly seen in PCOS
AFC is particularly useful in predicting ovarian response during IVF stimulation and is often used together with AMH to guide treatment planning.
AMH, AFC, and the POSEIDON Criteria
Modern fertility medicine increasingly uses the POSEIDON (Patient-Oriented Strategies Encompassing Individualized Oocyte Number) criteria, which classify patients with low ovarian reserve based on age, AMH levels, and AFC. This system helps doctors individualize treatment strategies and better estimate prognosis in women with reduced ovarian reserve.
By combining age, AMH, and antral follicle count, clinicians can predict ovarian response more accurately and tailor stimulation protocols accordingly.
Final Thoughts
AMH testing and antral follicle count are the two most important tools used today to evaluate ovarian reserve. While neither test measures egg quality directly, together they provide valuable information about reproductive potential and help guide fertility planning and treatment strategies.
For women considering pregnancy—especially those planning to delay childbearing—early evaluation of ovarian reserve can provide important insights and allow informed reproductive decisions.
References (Vancouver Style)
- Broekmans FJ, Soules MR, Fauser BC. Ovarian aging: mechanisms and clinical consequences. Endocr Rev. 2009.
- Practice Committee of the American Society for Reproductive Medicine. Testing and interpreting measures of ovarian reserve. Fertil Steril. 2020.
- La Marca A, Sunkara SK. Individualization of controlled ovarian stimulation in IVF using ovarian reserve markers. Hum Reprod Update. 2014.
- Poseidon Group. Patient-oriented strategies for individualized oocyte number in IVF: the POSEIDON criteria. Hum Reprod. 2016.
- Dewailly D, et al. Definition and significance of polycystic ovarian morphology. Hum Reprod Update. 2014.
- Tal R, Seifer DB. Ovarian reserve testing: clinical applications. Clin Obstet Gynecol. 2017.
